Types of Disease Transmission
Ever notice how a cold seems to travel from one person to another? First, your friend gets sick. Then, your friend’s sister gets sick. Next, her best friend gets sick. Eventually, half the class is suffering with the same symptoms. When a disease outbreak affects many people, it is called an epidemic. The word “epidemic” comes from the Greek words meaning “common among the people”. When this common sickness grows to global proportions it is called a pandemic.
In the 16th century, most people believed that disease was spread by foul air. There were no microbes, germs, or viruses – just air that had lost its ability to keep people healthy. So strong was this belief, that the Italian phrase for bad air, “malaria” was used to identify a common blood disease.
In 1546, a revolution occurred. In a work entitled “On Contagion”, Girolamo Francastoro proposed controversial beliefs on the spread of disease. He suggested that illness could be spread by a disease agent. Fracastoro argued that air transferred unseen agents from the infected to uninfected individuals. The infection progressed into a sickness that was accompanied by disease symptoms.
Laboratory data backing Francastoro’s work was slow to appear. It took unto 1870 for Louis Pasteur to fully present his convictions on microbes and disease. Pasteur’s beliefs, presented in his Germ Theory of Disease, implicated microbes as the cause of infectious disease.
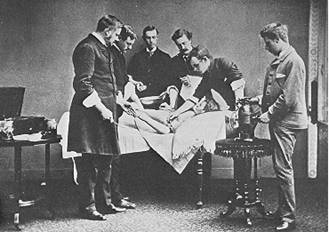
In the mid and late 1800s, recovery from major surgery wasn’t common. Although crude surgical procedures worked, the patients often died of infections - a common report by surgeons was: “operation successfully but the patient died”. Joseph Lister, an English surgeon, decided to improve his patients’ chances of recovery by sterilizing his instruments and disinfecting the operating room. These procedures used carbolic acid and heat to destroy populations of potentially fatal microbes. As expected, the recovery rate of Lister’s patients improved dramatically.
Ignatz Semmelweis was a Hungarian contemporary of Joseph Lister. Like  Lister, Semmelweis introduced the concept of sterilization and disinfection into the hospital environment. His actions were based upon the lower incidence of childbed fever in patients cared for by midwives. Semmelweis inferred that the midwives’ frequent hand washing reduced the spread of the disease. One day, Semmelweis and some of his colleagues were in the autopsy room performing autopsies as they often did between deliveries. One of Semmelweis’ friends was distracted by the conversation, and he punctured his finger with the scalpel. Days later, the man became sick, showing symptoms not unlike those of childbed fever. His friend’s ultimate death strengthened Semmelweis’ resolve to understand and prevent childbed fever. To improve hospital conditions, he required medical attendants to wash their hands in chlorinated lime. Although this procedure lowered the incidence of childbed fever, (mortality rates immediately dropped from 18.3% to 1.3%) it wasn’t popular among the staff. Semmelweis was ridiculed even with the overwhelming evidence and eventually dismissed from his position.
Lister, Semmelweis introduced the concept of sterilization and disinfection into the hospital environment. His actions were based upon the lower incidence of childbed fever in patients cared for by midwives. Semmelweis inferred that the midwives’ frequent hand washing reduced the spread of the disease. One day, Semmelweis and some of his colleagues were in the autopsy room performing autopsies as they often did between deliveries. One of Semmelweis’ friends was distracted by the conversation, and he punctured his finger with the scalpel. Days later, the man became sick, showing symptoms not unlike those of childbed fever. His friend’s ultimate death strengthened Semmelweis’ resolve to understand and prevent childbed fever. To improve hospital conditions, he required medical attendants to wash their hands in chlorinated lime. Although this procedure lowered the incidence of childbed fever, (mortality rates immediately dropped from 18.3% to 1.3%) it wasn’t popular among the staff. Semmelweis was ridiculed even with the overwhelming evidence and eventually dismissed from his position.
While Lister was sterilizing scalpels, and Semmelweis was washing hands, Robert Koch was studying the spread of anthrax and tuberculosis. From his observations, Koch compiles a set of postulates that would guide others in the study of infectious disease. These steps outlined the procedure for uncovering an agent of disease. These rules, which were presented formally in 1878, became known as Koch’s Postulates. They state:
1. The suspect microbe must be present in the diseased animal
2. The suspect microbe must be isolated from the diseased animal and grown in pure culture
3. When the microbes obtained from the pure culture are introduced into a healthy animal, the animals must become diseased.
4. Microbes from the new host must be removed and compared with the suspect original microbes to confirm its role in disease.
Adapted from “The Science of HIV”
Name:_____________________________________________________
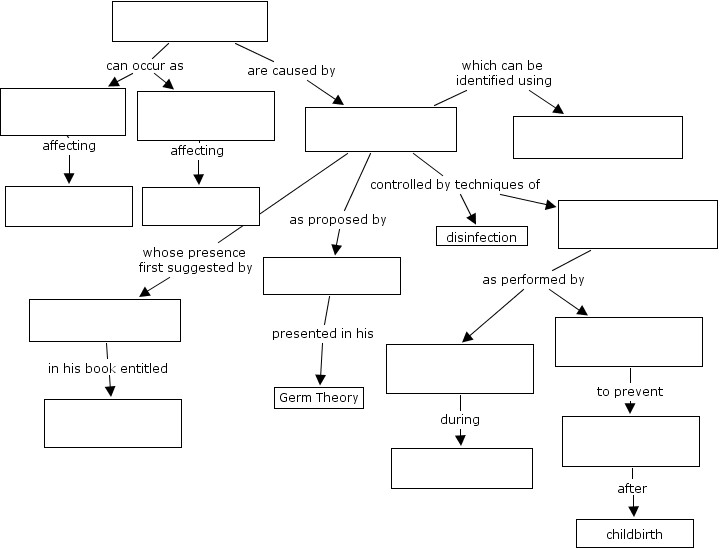
CONCEPT MAP